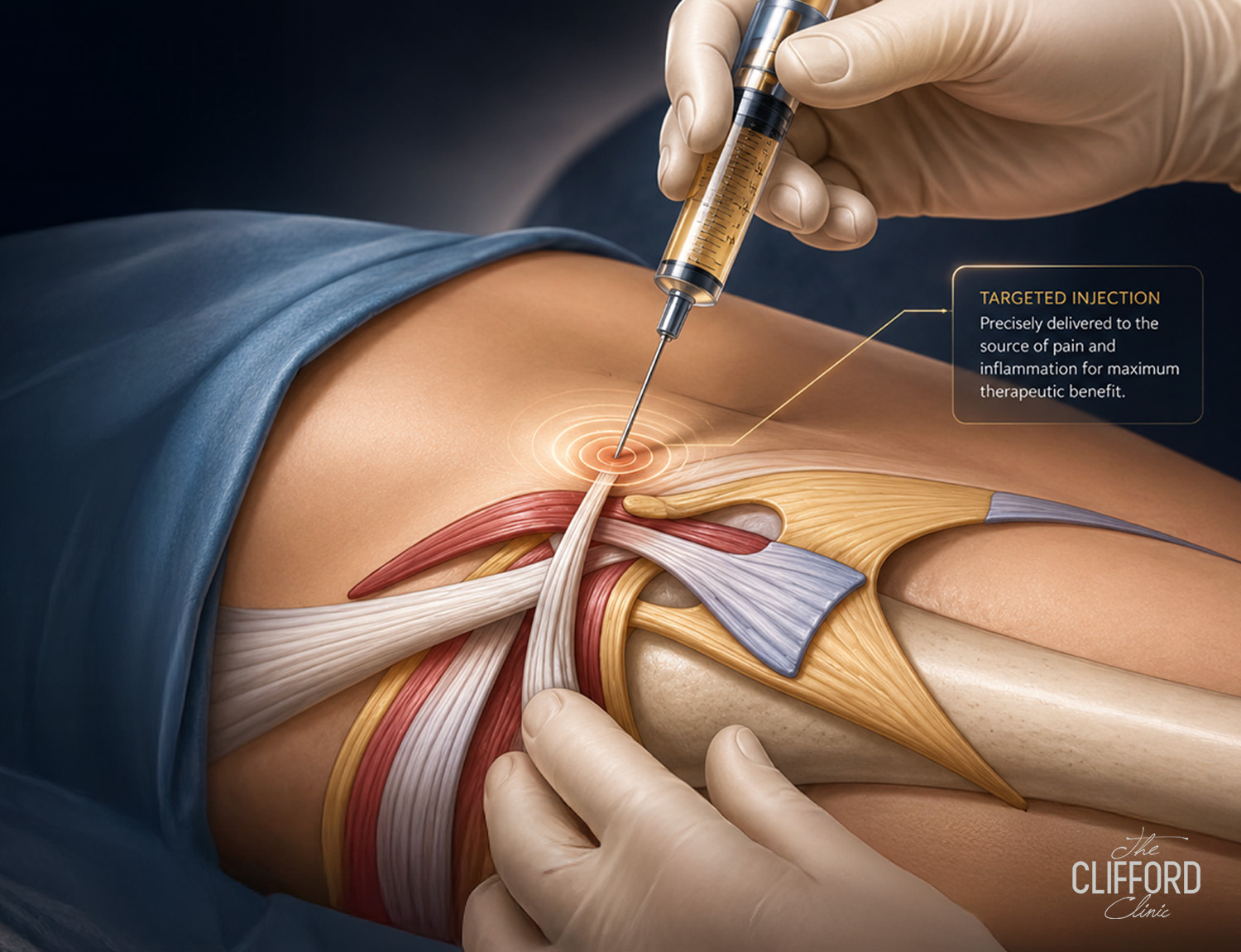
Prolotherapy for Tendon Injuries: 2026 Doctor’s Complete Guide to Dextrose Prolotherapy for Tendinopathy
Tendon injuries are frustrating because they rarely behave like simple muscle strains.
A tendon can stay painful for months, flare with training, settle with rest and then return the moment you load it again. This pattern is common in tendinopathy, a broad term for chronic tendon pain and reduced tendon function that often develops from repeated overload rather than a single traumatic event.
Prolotherapy is an injection option that some clinicians use for chronic musculoskeletal pain, including certain tendon and attachment site problems. The most common form is dextrose prolotherapy, where a small amount of concentrated dextrose solution is injected into painful tissues such as tendons, ligaments or joint-related soft tissue, with the goal of stimulating a local healing response. At the same time, reputable medical sources note that evidence is mixed, that results can be inconsistent and that the treatment is not a standard first-line option for most conditions.
This comprehensive guide focuses on prolotherapy for tendon injuries across the body, including rotator cuff pain, tennis elbow, golfer’s elbow, patellar tendon pain, Achilles pain and plantar fascia pain. It outlines how the team at The Clifford Clinic approaches prolotherapy for tendon-related pain through careful diagnosis, ultrasound guidance when appropriate and structured rehabilitation support, without making exaggerated claims or guarantees.
Understanding tendon injuries and tendinopathy
Many people use the word tendinitis to describe tendon pain. In practice, persistent tendon pain often involves more than inflammation. Over time, a tendon can develop changes in collagen structure and pain sensitivity, leading to reduced load tolerance. This is why you can feel pain with stairs, running, jumping or lifting even when there is no major tear.
Tendinopathy typically causes chronic pain and reduced function in the affected tendon.
A key point is that tendinopathy is usually managed with graded loading. That means progressive strengthening and carefully controlled exposure to activity. Injections, when used, are usually considered an adjunct to help pain and function while rehabilitation addresses the underlying capacity and biomechanics that contributed to the injury.
What is prolotherapy
Prolotherapy is an injection treatment in which a clinician injects a small amount of an irritant solution into painful connective tissue. Dextrose solution is the most commonly injected irritant in modern prolotherapy. The treatment is used for musculoskeletal conditions involving bones, muscles, tendons, ligaments and soft tissues.
Prolotherapy is often described as an elective option. It is not considered a cure for tendinopathy or any other condition. Medical sources emphasise that results vary, that research is not conclusive and that some benefits reported in studies may be influenced by placebo response and other contextual factors.
How prolotherapy is thought to work
The proposed idea is that injecting concentrated dextrose into a targeted region creates a controlled local irritant effect. In theory, this signals the body to increase local healing activity in that area.
This is an attempt to jump-start the body’s healing response, although they also note that scientifically significant proof of the exact mechanism is limited.
For tendon problems, the clinical aim is often practical rather than theoretical. Identify the painful portion of the tendon or its attachment site, treat it precisely and then support recovery with a progressive loading plan. The injection alone is rarely the full solution.
What tendon injuries can prolotherapy be used for
Prolotherapy is discussed in a range of chronic overuse conditions. In tendon-focused practice, it is most commonly considered for tendinopathy and enthesopathy, meaning pain where a tendon attaches to bone.
Common tendon and related conditions where prolotherapy has been studied or discussed include:
1. Rotator cuff tendinopathy
Shoulder pain often worsened by overhead activity, lifting or sleeping on the affected side. A sports medicine review discussing prolotherapy includes rotator cuff tendinopathy among conditions commonly addressed in prolotherapy literature.
2. Lateral epicondylosis and medial epicondylosis
These are commonly known as tennis elbow and golfer’s elbow. Evidence includes randomised trials and systematic reviews evaluating dextrose-based prolotherapy and related injection approaches for lateral elbow tendinopathy.
3. Patellar tendinopathy
Often called jumper’s knee, this causes pain at or just below the kneecap that worsens with stairs, squats, jumping or running. A 2024 systematic review on prolotherapy in tendinopathies includes patellar tendinopathy among the common conditions studied.
4. Achilles tendinopathy
Pain and stiffness at the Achilles tendon, often worse with running, jumping and morning steps. A systematic review of dextrose prolotherapy for chronic musculoskeletal pain includes Achilles tendinopathy among conditions with reported improvements in some studies, while also highlighting that evidence quality varies.
5. Plantar fascia pain and plantar fasciopathy
Heel pain from plantar fascia overload is commonly studied in prolotherapy literature. A 2023 systematic review evaluated hypertonic dextrose prolotherapy for plantar fasciopathy compared with other non-surgical treatments.
6. Iliotibial band-related pain and lateral knee pain patterns
The IT band is a fascia-like structure rather than a tendon, but it behaves like an overuse load problem and is often discussed alongside tendinopathy. In practice, treatment still relies heavily on load management and strength, with injections considered selectively.
Who may benefit
You may be a candidate for prolotherapy if your clinician has identified a tendon or attachment site problem that has not improved despite a proper rehabilitation plan. In general, prolotherapy is most often discussed for persistent pain, recurrent flare-ups with loading and conditions where conservative care has been tried consistently.
Your clinician may discuss prolotherapy if you have one of these conditions or patterns, with the most tendon-relevant group listed first:
-
Tendinopathy including rotator cuff, lateral epicondylosis, medial epicondylosis, patellar tendinopathy, Achilles tendinopathy and certain overuse pain patterns affecting the IT band region
-
Plantar fasciopathy and chronic heel pain
-
Osgood-Schlatter related pain in appropriate contexts
-
Chronic back pain and sacroiliac region pain in selected cases, noting that evidence and protocols vary across studies
-
Osteoarthritis pain affects joints such as the knee, ankle, foot, shoulder, elbow, fingers or hip, though major guidelines recommend against routine prolotherapy for knee and hip osteoarthritis due to limited trials and heterogeneity
-
Chronic groin pain in athletes, TMJ pain and hypermobility-related pain, where evidence may be more variable and selection becomes especially important
The most important message is that prolotherapy should match the diagnosis. Tendon pain from overload behaves differently from pain driven by a full-thickness tendon tear, mechanical impingement or joint instability.
Who may not be suitable
A careful clinician will screen for situations where prolotherapy is unlikely to help or may be unsafe. Common reasons to avoid or defer include:
- Active infection at the skin or systemically
- Unclear diagnosis where the pain generator has not been identified
- Suspected complete tendon rupture or a tear pattern that needs a different treatment pathway
- High bleeding risk or anticoagulant issues that cannot be managed safely
- Known allergy to any component used in the procedure
- Medical instability where elective procedures should be postponed
It is also important to recognise when a tendon injury is not the main problem.
For example, shoulder pain can come from the rotator cuff, the joint capsule or nerve-related causes.
Elbow pain can come from tendon overload, nerve irritation or referred pain. A diagnosis-first approach reduces the risk of treating the wrong structure.
Prolotherapy for knee tendon injuries
Knee pain is often assumed to be joint cartilage or meniscus-related, but a large proportion of persistent knee pain in active people is driven by tendon overload around the kneecap. The most common tendon patterns are patellar tendinopathy which is pain at or just below the kneecap and quadriceps tendinopathy which is pain above the kneecap.
These usually feel load-related, meaning symptoms flare with stairs, squats, lunges, jumping and running. The pain is often localised and easy to point to with one finger rather than a vague ache throughout the whole knee.
Before prolotherapy is considered, the key step is confirming that the primary pain generator is tendon-based and not something else. A good assessment looks at your training load and movement patterns, checks strength and biomechanics at the hip, knee and ankle and considers imaging when it helps clarify the diagnosis.
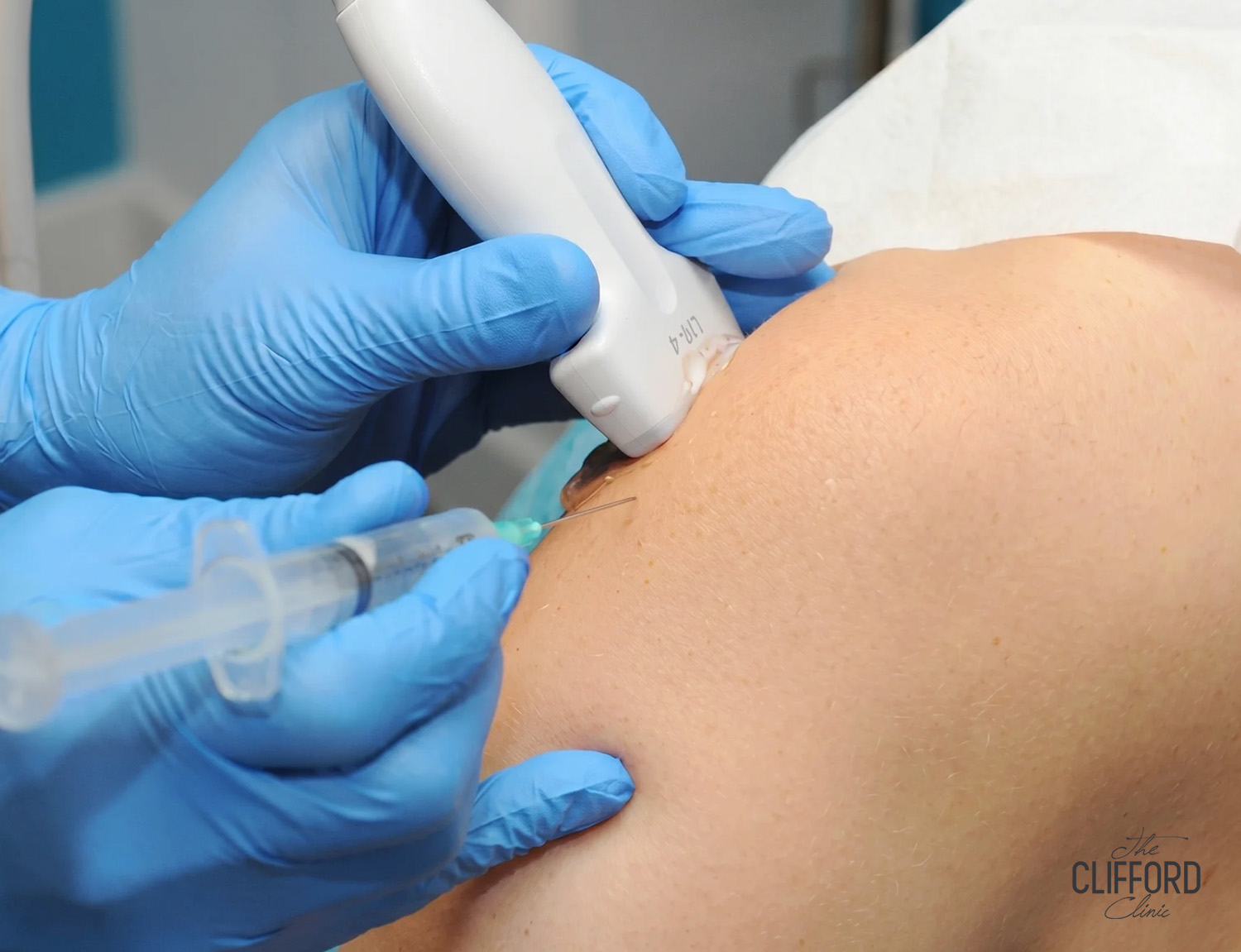
Ultrasound can be useful to evaluate tendon structure and to help guide injection placement when appropriate. This step matters because prolotherapy is not designed to treat every cause of knee pain, so ruling out issues like significant joint arthritis, mechanical meniscus symptoms or instability changes the treatment plan.
When prolotherapy is used for knee tendon pain, it is typically positioned as an adjunct to rehabilitation rather than a replacement for it. The injection plan is tailored to the clinical findings, then paired with a structured loading programme that rebuilds tendon capacity. After the procedure, it is normal to feel mild soreness for a few days and you are usually advised to avoid sudden high-impact loading early on, then progress gradually through strengthening before returning to running or sport.
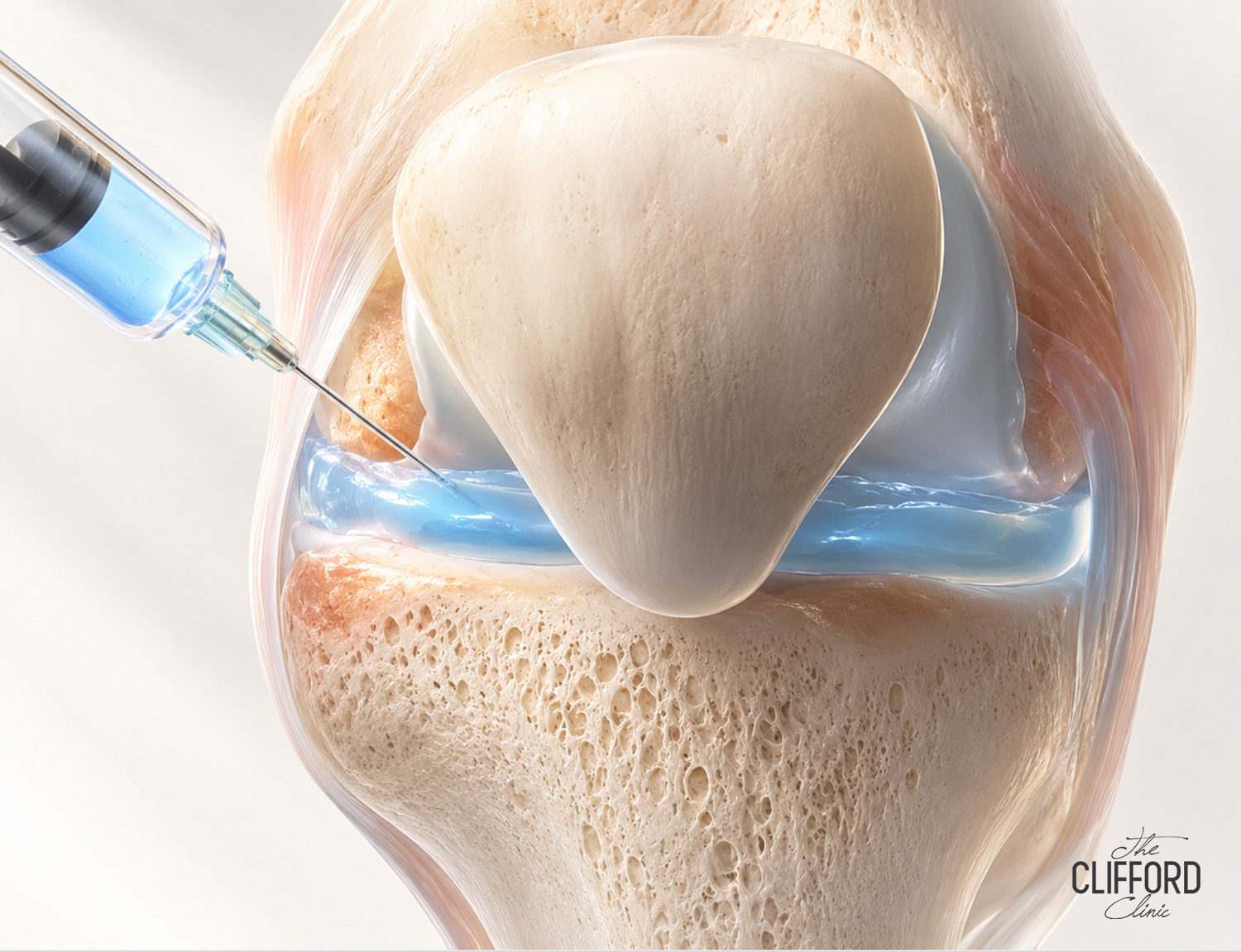
What happens during the procedure
During a prolotherapy session, your provider injects dextrose solution into joints, tendons or ligaments where you are experiencing pain. Ultrasound guidance may be used depending on the target.
While protocols vary, the procedure usually follows a consistent flow:
- First, the skin is cleaned and sterile technique is used.
- Next, the clinician identifies the target structure by exam and when used by ultrasound.
- Then, the dextrose solution is injected into the planned sites.
- Afterwards, you receive aftercare instructions and a plan for follow-up.
A practical detail many people want to know is the number of sessions. Medical sources describe that people usually need several sessions and may receive a total of three to six injections over the course of their prolotherapy sessions, depending on the body region and the clinician’s plan.
What to expect after prolotherapy
Many people can return to daily activities quickly, but it is common to feel soreness at the injection site for a short period. Medical sources describe little to no recovery time for daily activities, while advising patients to speak with their provider before resuming intense workouts or sports after an injection.
For tendon injuries, aftercare should be paired with a clear rehabilitation plan. The core principle is graded loading. Tendons need load to recover, but the load must be progressed gradually to avoid flare-ups.
A sensible plan often includes an early period of relative rest from high-impact triggers, followed by progressive strengthening and then return to sport progression.
Benefits and limitations of tendon injuries
When prolotherapy helps tendon injuries, the benefit is usually felt as improved ability to tolerate loading, reduced pain during daily tasks and better return to training progression. It is minimally invasive and can be combined with other treatments and rehabilitation.
The limitations are equally important. Research has found inconclusive results overall and that improvements may be influenced by placebo effects and other factors. Treatment protocols vary widely across studies, which makes it difficult to compare outcomes directly across conditions.
For this reason, prolotherapy is best framed as an option to consider in selected cases, especially when conservative care has been attempted properly and goals are clear.
What the research suggests for tendon conditions
The evidence base for prolotherapy in tendinopathy is growing but heterogeneous. A 2016 systematic review examined dextrose prolotherapy across chronic musculoskeletal pain conditions and included tendinopathy presentations, while also noting variation in study design and evidence levels.
For lateral elbow tendinopathy, evidence includes both clinical trials and systematic reviews. A 2013 randomised trial reported significant improvements in elbow pain and function compared with a wait-and-see control group. A 2022 systematic review and meta-analysis found hypertonic dextrose prolotherapy was superior to active controls at around 12 weeks for pain and function in lateral elbow tendinopathy, while also noting that study sizes were small and rare adverse events could not be assessed well.
For plantar fasciopathy, a 2023 systematic review evaluated hypertonic dextrose prolotherapy compared with other non-surgical treatments. A 2023 meta-analysis also reported overall short-term improvements in pain and function compared with placebo or other non-surgical interventions, with significant heterogeneity across included studies.
A 2024 systematic review focused specifically on prolotherapy in tendinopathies described prolotherapy as a promising alternative, while also reflecting that protocols and evidence quality vary across conditions.
The practical takeaway is that prolotherapy may be worth discussing for some tendon conditions, especially those that have not responded to first-line care, but it should be presented with realistic expectations and clear alternatives.
Prolotherapy compared with other tendon treatment options
For tendon injuries, the foundation is still a structured rehabilitation programme. Beyond that, clinicians may discuss adjunct options depending on the diagnosis.
- Physiotherapy and progressive loading remain central for most tendinopathy.
- Shockwave therapy is commonly used for conditions such as plantar fascia pain and certain tendon problems.
- Corticosteroid injections may reduce pain short term in some conditions but can be less suitable for certain chronic tendon presentations depending on location and goals.
- PRP is used in some tendon conditions, but evidence and standardisation vary by body region and protocol.
- Percutaneous procedures such as ultrasonic tenotomy are used in selected chronic tendon cases where removing degenerative tissue is a goal.
The right option depends on tendon location, severity, imaging findings, time course and the quality of prior rehabilitation.
How to choose a clinic for prolotherapy for tendon injuries
Because prolotherapy is technique-dependent, selection should focus on process rather than promises.
A clinic should be able to explain the diagnosis clearly, including why the problem is tendon-related. They should outline the plan for rehabilitation, because tendon improvement depends heavily on load management and progressive strengthening.
If ultrasound guidance is used, the clinician should have competence in musculoskeletal ultrasound assessment and procedural guidance. Medical sources describing prolotherapy explicitly note that ultrasound may be used to guide injections.
The clinic should also be transparent about uncertainty. Prolotherapy may help, may do nothing or may provide temporary improvement. Reputable sources emphasise that evidence is inconclusive and that effectiveness is debated.
Prolotherapy for tendon injuries at The Clifford Clinic
At The Clifford Clinic in Singapore, prolotherapy is approached through diagnosis first, careful target selection and structured rehabilitation support. The intent is to offer prolotherapy as one possible option for selected tendon injuries, without overselling results.
The consultation focuses on confirming whether your pain pattern fits a tendon or attachment site problem and whether conservative management has been adequate.
Ultrasound may be used when it improves diagnostic clarity or procedural accuracy, especially for tendon targets where image guidance can support precision.
Aftercare is planned around a staged return to loading. Tendons respond to gradual progression, so the goal is to help you return to activity with fewer flare-ups by combining any injection plan with rehabilitation and load management.
If you are exploring prolotherapy for tendon injuries, a consultation at The Clifford Clinic can help clarify whether prolotherapy fits your diagnosis, what alternatives exist and what a realistic recovery plan should look like.
Frequently asked questions
Does prolotherapy cure tendinopathy
No. Prolotherapy is an injection option aimed at pain management and potential functional improvement. It should not replace rehabilitation and it is not described as a cure for any condition.
How many sessions are needed
Protocols vary. Some sources describe that people usually need several sessions and may receive a total of three to six injections across the course of treatment.
Can it be done with other treatments
Yes, it is often considered alongside rehabilitation. Medical sources describe that it can be used with other treatments, with the caution that you should discuss the full plan with your clinician.
When can I return to sport
Return depends on the tendon, the severity and how your rehab progresses. Your provider should give a staged plan. In general, tendons need gradual reloading rather than sudden return to maximal activity.
Summary
Prolotherapy most commonly involves injecting dextrose solution into painful connective tissue such as tendons, ligaments and joint-related soft tissue. For tendon injuries, prolotherapy is discussed as an adjunct option for selected chronic cases, often alongside progressive strengthening and load management.
References
-
Systematic review of dextrose prolotherapy for chronic musculoskeletal pain including tendinopathy discussions and evidence limitations.
-
Randomised trial of prolotherapy for lateral elbow tendinopathy reporting improvement in pain and function versus control.
-
Systematic review and meta-analysis for hypertonic dextrose prolotherapy in lateral elbow tendinopathy reporting short-term improvements.
-
Systematic review of hypertonic dextrose prolotherapy in plantar fasciopathy.
-
Meta-analysis on dextrose prolotherapy for chronic plantar fasciitis reporting short-term benefits with heterogeneity.
-
Systematic review of prolotherapy in tendinopathies summarising emerging evidence across common tendon conditions.
-
Review discussing prolotherapy in sports-related musculoskeletal conditions including rotator cuff tendinopathy, plantar fascia pain and Osgood Schlatter disease.