
Knee Joint Injection in Singapore: A Practical, Research-Driven Guide
Introduction
If knee pain has begun to set the rhythm of your day—slowing the morning walk, making MRT stairs feel longer, or turning a hawker-centre meal into a search for the nearest seat—you’re not alone. Across Singapore, active adults, weekend tennis players, joggers on the East Coast Park route, and caregivers on their feet all day face the same problem: the knee aches, swells, and stiffens. When rest, ice, and tablets only help a little, doctors often suggest a knee joint injection to calm things down so you can move again. In this guide, you’ll get a clear, down-to-earth explanation of which injections are used, how the procedure feels, what results to expect, and how to make relief last. You’ll also see how a research-anchored approach—exemplified by Singapore Dr Gerard Ee, whose work appears in top-tier journals including Knee—turns precision into everyday results for patients.
What a Knee Joint Injection Is—and Who Usually Benefits
A knee joint injection is a targeted treatment delivered into the knee’s intra-articular space to reduce pain, ease inflammation, and improve movement. It’s commonly recommended for osteoarthritis, which is the gradual thinning and fraying of cartilage cushioning the ends of the femur and tibia. In Singapore clinics it’s also used for patellofemoral pain linked to maltracking, meniscal wear-and-tear that triggers synovial irritation, and inflammatory flare-ups that make the joint hot and tight.
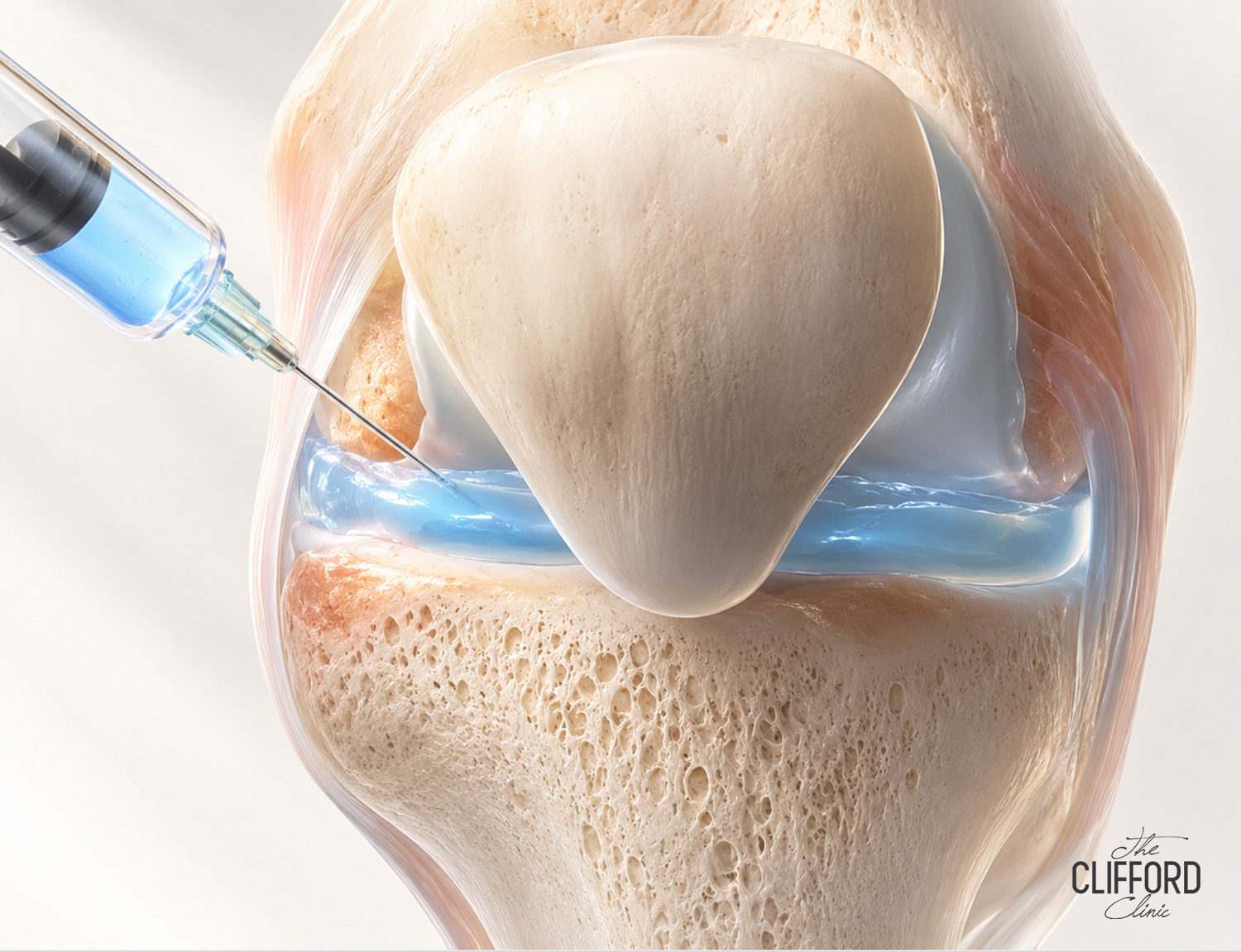
You may be a good candidate if pain flares with walking or stairs, if swelling limits your bend, or if night aches disrupt sleep. Injections can be particularly helpful when discomfort makes it hard to do the very physiotherapy exercises that protect the knee long-term. Think of the injection as a bridge: it lowers pain enough for you to rebuild strength and confidence without gritting your teeth through every rep.
There’s a common question in Singapore: “Isn’t an injection just a quick fix?” The honest answer is that it’s a useful tool, not a magic wand. The best results happen when an injection is paired with a plan—graded activity, targeted physiotherapy, footwear or orthotic tweaks that improve alignment, and (where relevant) weight management to reduce load on the joint. Used this way, a knee joint injection is often the nudge that gets a stuck knee moving again.
The Main Types You’ll Hear About—and When Each Makes Sense
In real-world practice, three options cover most needs.
Corticosteroid injections are anti-inflammatory. When a knee is swollen, irritable, and warm, steroids are often the fastest way to break that cycle. Relief can start within days and last weeks to a few months. They’re especially useful to calm an acute flare so you can start physiotherapy. Because steroids can nudge blood sugar, patients with diabetes are advised on timing, monitoring, and safe frequency.
Hyaluronic acid injections—also called viscosupplementation—aim to restore some of the knee’s natural lubrication. Patients usually describe the benefit as smoother movement rather than an instant “switch-off” of pain. Effects tend to build gradually and can last several months in suitable knees. In Singapore, hyaluronic acid is commonly offered to active adults and seniors with mild-to-moderate osteoarthritis who find stairs, slopes, or longer walks increasingly limiting.
Platelet-rich plasma Injection (PRP) comes from your own blood, concentrating platelets that release growth factors. People who choose PRP injections often want to minimise steroid exposure or prefer a biologic option. Response varies, and the gains are typically about improved tolerance for everyday activity rather than a dramatic overnight change. The key is matching the option to your knee’s biology and your goals—chasing trends rarely beats tailoring the plan.
It’s worth saying: the “best” injection is the one that fits your diagnosis, timing, and rehab pathway. Experienced teams in Singapore will explain why they’re recommending a particular choice rather than defaulting to a one-size-fits-all protocol.
What to Expect Before, During, and After
A focused assessment comes first. That usually includes a careful history, hands-on examination, and—when useful—imaging such as X-rays or MRI to confirm whether pain arises from joint surfaces, the patellofemoral groove, meniscal degeneration, or referred sources like the hip or lumbar spine. Aligning diagnosis with treatment is the step that most influences results.
The procedure itself is straightforward. The skin is cleaned, local anaesthetic may be used to numb the area, and the needle is introduced into the joint space. Many specialists in Singapore use ultrasound guidance to improve accuracy and comfort; patients often describe a brief pinch and pressure rather than sharp pain. The injection takes minutes, and you can usually walk out of the clinic.
For the next day or two the knee can feel heavy or full, particularly after hyaluronic acid or PRP. That typically settles with ice, relative rest, and simple analgesics. Most desk workers return the same day; light exercise resumes as comfort allows. The follow-through matters: clinics often schedule a short review to track pain scores, range of motion, and progress with physiotherapy. Small milestones—restoring extension, flexion beyond 120 degrees, and single-leg control—translate into everyday wins like taking the overhead bridge near the MRT without stopping or finishing a loop at Gardens by the Bay without clock-watching.
Results You Can Expect—and How to Make Them Last
Two questions come up in almost every consult: how soon will it help, and how long will it last? Steroid relief is the quickest, often within days, and can last weeks to a few months. Hyaluronic acid builds more gradually and can smooth movement for several months in appropriate knees. PRP benefits vary; many patients notice sturdier day-to-day function rather than a dramatic overnight shift. These are averages. Your cartilage health, alignment, activity goals, and commitment to rehab all influence the curve.
Practical insights from Singapore practices are consistent. First, the biggest gains happen when the injection unlocks physiotherapy, not replaces it. Once pain settles, people can tolerate the quad and hip strengthening that offloads the knee—especially the medial compartment that tends to bear the brunt during common Asian lifestyle movements like deep knee bends. Second, pacing matters. Knees prefer steady progress to weekend surges. Third, tiny form tweaks—avoiding knee-in collapse on stairs or during squats—cut down patellofemoral irritation and extend your “good knee days.”
A composite example reflects what many patients experience. Picture a 62-year-old retiree who loves brisk morning walks along the Kallang River. Medial knee pain starts to limit her loop, and she begins to avoid stairs at her HDB block. X-rays show moderate medial compartment osteoarthritis. A carefully chosen knee joint injection calms the flare, and she begins guided physiotherapy within a week, focusing on quadriceps endurance, gluteal strength, and step-down control. Three months later, she’s comfortably back to 45 minutes at East Coast Park and taking the MRT stairs without a pause. The injection opened the door; the right exercises kept it open.
Safety, Side Effects, and How Risk Is Minimized
No medical procedure is risk-free, and injections should be approached with honesty and care. The most common transient effects are local soreness, a sense of fullness in the joint, and minor bruising at the needle site. Joint infection is rare but serious; sterile technique, a clean environment, and careful screening keep that risk very low. People with diabetes should know that corticosteroids can temporarily raise blood glucose, so timing is coordinated and readings are monitored. Patients on blood thinners usually can proceed with appropriate precautions, but the specifics are individual. Allergy to local anaesthetic or the injection material is uncommon, but it’s always checked for in advance.
Frequency matters as well. Steroid injections are typically spaced to avoid over-reliance, and decisions about repeating them weigh pain relief against overall joint health. Hyaluronic acid and PRP schedules vary by product and by the knee’s condition; reputable clinicians will explain why a particular plan makes sense for you.
Ultrasound guidance can improve accuracy and reduce the number of needle passes, which helps comfort. Just as important is matching the injection to the patient: the best outcomes happen when the right pain generator is treated at the right moment, with a clear plan for what comes next.
When Injections Aren’t Enough: Precision, Surgery, and Why Research Matters
Most people in Singapore understandably want to avoid surgery, and many can. When injections unlock progress and physiotherapy anchors it, a large share of patients return to their chosen activities without ever seeing an operating theatre. But it’s equally important to recognize when structural issues—significant bow-leg or knock-knee alignment, global cartilage loss, or mechanical symptoms from complex meniscal tears—push a knee past the tipping point.
That doesn’t negate the value of injections. It clarifies their role within a broader, staged plan. In the surgical pathway, an injection may settle inflammation so you can complete pre-hab, or keep you mobile while deciding on the timing of a partial or total knee replacement.
This is where meticulous, research-driven thinking matters. Dr Gerard Ee co-authored a paper in Knee—“Computer navigation is a useful intra-operative tool for joint line measurement in total knee arthroplasty” (2013;20(4):256-62; Epub 2012 Dec 7; doi:10.1016/j.knee.2012.10.026)—with colleagues Hee Nee Pang, Hwei Chi Chong, Mann Hong Tan, Ngai Nung Lo, and Seng Jin Yeo. The study prospectively analysed 168 computer-assisted total knee arthroplasties and found that larger changes in the joint line, particularly outliers of ≥4 mm, were associated with poorer outcome scores, highlighting why joint-line precision influences function after TKA. That same precision-first mindset carries into non-operative care, informing where to inject, how to interpret imaging, and how to stage a plan that moves logically from injection to rehabilitation—or, when necessary, to surgery with well-defined goals.
Why Many Singapore Patients Choose Dr Gerard Ee

In healthcare, who you see matters as much as what you get. Dr Gerard Ee’s publication record in respected orthopaedic journals reflects a career shaped by data, careful technique, and measurable outcomes. His paper in Knee on computer-navigated joint-line assessment has become a useful reference for understanding why millimetres matter when aligning the knee. That mindset translates directly to the clinic: using ultrasound guidance to confirm accurate needle placement, tailoring injection choice to cartilage patterns seen on imaging, and building a month-by-month plan that links the procedure to physiotherapy milestones you can actually achieve. Patients value clear explanations, realistic timelines, and a plan that respects Singapore’s active lifestyles—from returning to Dragon Boat training without swelling after every session to walking the Bishan-Ang Mo Kio Park loop with grandkids without thinking about your knees.
Costs, Logistics, and What to Ask at Your Visit
Fees vary with the type of injection, whether ultrasound guidance is used, and the clinical setting. Instead of focusing on a headline number, ask for an itemised plan: what result is expected for your specific diagnosis, how the injection integrates with physiotherapy, how many injections are typically considered before switching strategies, and when your progress will be reviewed. Singapore clinics are generally transparent about billing and can advise on insurance coverage; a short conversation prevents surprises later.
Preparation is simple. Wear clothing that allows easy access to the knee. Eat normally unless advised otherwise. Bring a list of medications and supplements, and mention any prior reactions to injections or local anaesthetics. Plan your day so you’re not rushing from the clinic to a high-impact workout; most people walk out comfortably and return to desk work the same day. Book your first physiotherapy session within one to two weeks after the injection so momentum is built in from the start. Success is rarely accidental—it’s arranged.
Conclusion — Your Next Step
Pain that limits your life is not a price you have to pay. If you’re considering a knee joint injection, choose a team that treats precision as a habit and not a slogan. In Singapore, clinicians like Dr Gerard Ee bring research-tested thinking and calm, patient-first care to an option that too often is treated as a quick jab and goodbye. When injections are matched to your knee and paired with a realistic rehab plan, they can reduce pain, restore confidence, and give you back ordinary joys like stairs, unhurried walks, and uninterrupted sleep.
If your knee has been calling the shots, it’s time to take the next step. Arrange a consultation in Singapore to determine whether a knee joint injection is appropriate for you, how it would fit into a broader plan, and what results you can reasonably expect. A short, informed appointment can change the course of your year.
Frequently Asked Questions
Is the injection painful, and how long does it take?
Most people describe a brief pinch followed by pressure rather than sharp pain. Local anaesthetic can be used to numb the skin, and ultrasound guidance helps position the needle accurately. The injection itself usually takes minutes, and you can typically walk out of the clinic right away. Mild soreness or fullness for a day or two is common and settles with ice, relative rest, and simple analgesics.
How soon will I feel better, and how long does relief last?
Timing depends on the material and your knee’s condition. Corticosteroids can calm a flare within days and reduce pain for weeks to a few months. Hyaluronic acid tends to build gradually and can smooth movement for several months in suitable knees. PRP varies between individuals. Regardless of type, the most durable improvements happen when the injection opens the door to physiotherapy and better movement habits rather than attempting to replace them.
Can I have a knee joint injection if I have diabetes or take blood thinners?
Many patients with these conditions do proceed safely, but the plan is personalised. Steroids can transiently raise blood glucose, so timing and monitoring are coordinated for people with diabetes. Blood thinners usually do not rule out injections, yet precautions are taken and decisions are made in partnership with your clinician. Always share your full medication list and medical history so your team can prepare appropriately.
Medical information here is general and does not replace personalised advice. For recommendations specific to your knee, please consult an orthopaedic specialist in Singapore.



