
HA and PRP Knee Injections
Recent advances in intra-articular injection therapies for knee joint pathology have focused on biologic agents, particularly hyaluronic acid (HA) and platelet-rich plasma (PRP). These modalities are most extensively studied in knee osteoarthritis (OA), with emerging but less robust data for ligamentous, meniscal, and cartilage defects.
Knee Osteoarthritis: Comparative Efficacy
Multiple meta-analyses and systematic reviews demonstrate that PRP injections provide superior long-term pain relief and functional improvement compared to HA for mild to moderate knee OA. PRP consistently outperforms HA in Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC), Visual Analog Scale (VAS), and International Knee Documentation Committee (IKDC) scores at 6–12 months post-injection. The American Academy of Orthopaedic Surgeons guideline notes that PRP maintains improvement beyond 6 months, whereas HA’s effect wanes after this period. PRP preparation methods matter: leukocyte-poor PRP is associated with better outcomes than leukocyte-rich PRP.
Combination Therapy: PRP + HA
Recent meta-analyses and randomized trials have evaluated the efficacy of PRP plus HA compared to monotherapy. The most up-to-date evidence indicates that:
- PRP + HA is superior to HA alone for pain reduction and functional improvement at 3, 6, and 12 months, as measured by VAS and WOMAC scores. For example, Karasavvidis et al. found that PRP+HA resulted in significantly greater improvements in VAS at all time points and in WOMAC physical function and stiffness at 12 months compared to HA alone.
- PRP + HA may offer incremental benefits over PRP alone in some studies, particularly for pain reduction at 6 and 12 months, but the magnitude of difference is modest. Liu et al. (2025) reported that PRP+HA achieved better long-term pain relief and functional improvement than PRP alone, with a lower risk of adverse events.
- Other randomized trials and systematic reviews have found no statistically significant difference between PRP+HA and PRP alone for most functional outcomes at 6 and 12 months. Fossati et al. (2024) showed comparable efficacy among PRP+HA, PRP, and HA for pain and function in mild to moderate OA.
- The sequence and timing of injections may influence outcomes, but optimal protocols remain undetermined. Most studies use three intra-articular injections spaced 1–2 weeks apart.
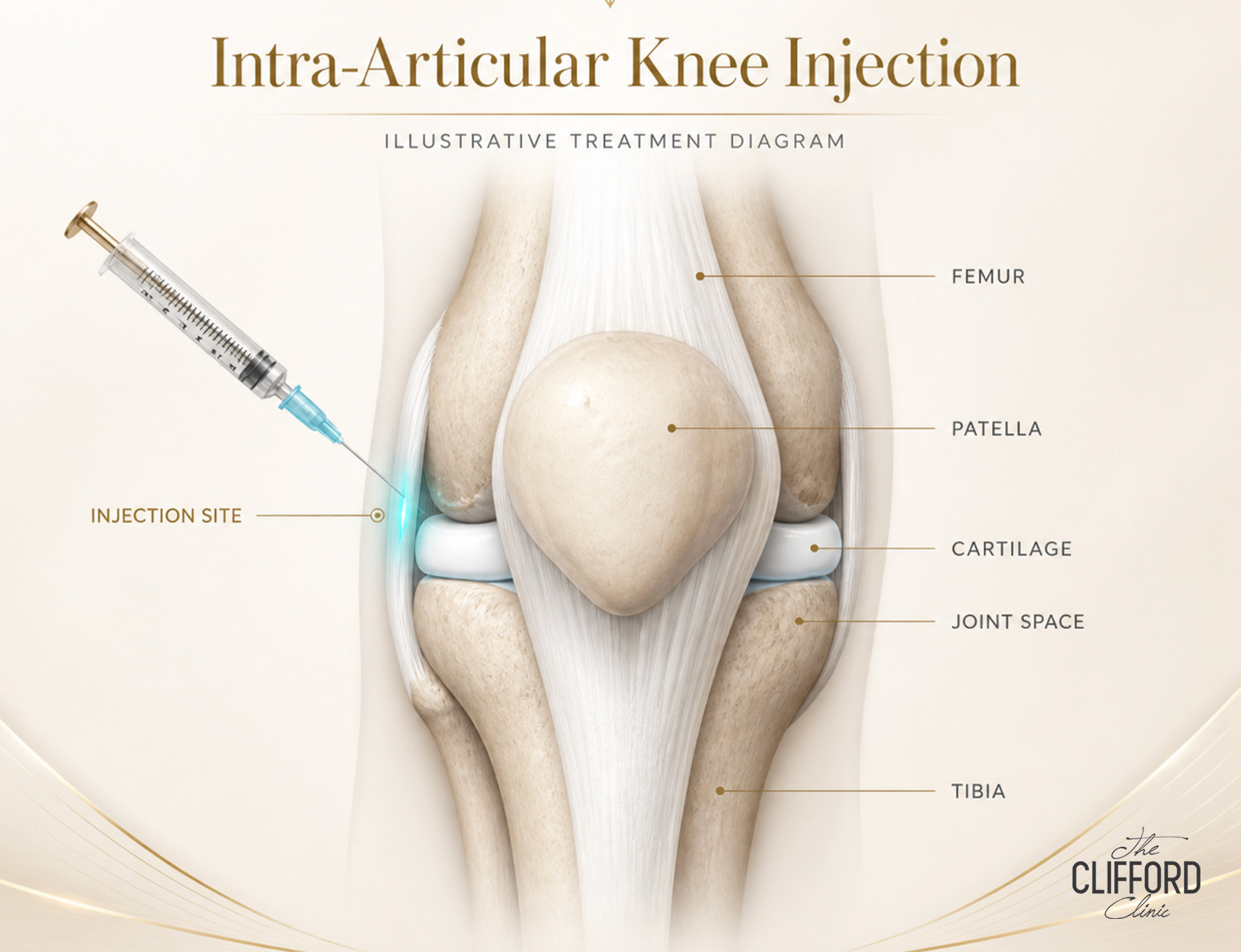
Procedural Considerations
PRP is typically administered as 1–3 intra-articular injections, often spaced 1–2 weeks apart. HA is commonly injected every six months for symptomatic OA.[6] Combination therapy protocols generally involve sequential or simultaneous administration, but further research is needed to standardize these approaches. The choice of PRP preparation (leukocyte-poor vs. leukocyte-rich) and HA formulation may impact outcomes.
Ligamentous, Meniscal, and Cartilage Defects
The evidence base for intra-articular HA and PRP in ACL, PCL, meniscus, and cartilage defects is limited. Most studies focus on OA-related pain and function, with few high-quality trials addressing isolated ligament or meniscal injuries. Current guidelines and meta-analyses do not support routine use of HA or PRP for acute or chronic ACL/PCL tears, meniscal injuries, or focal cartilage defects outside of OA. While preclinical and small clinical studies suggest potential benefits in tissue healing and symptom relief, robust randomized controlled trial data are lacking.
Clinical Practice Implications
For patients with symptomatic knee OA, PRP knee injection is the preferred injectable therapy, offering sustained pain relief and functional improvement. HA remains an option for those unable to access PRP or with contraindications. Combination therapy (PRP+HA) may be considered in select cases, particularly where enhanced pain relief or safety is desired, but the incremental benefit over PRP alone is modest and not consistently demonstrated across all studies. Routine use of PRP or HA for ligamentous, meniscal, or cartilage pathology is not supported by current evidence.
Limitations and Future Directions
Heterogeneity in PRP preparation, injection protocols, and patient selection limits direct comparison across studies. Further research is needed to clarify the role of biologic injections in non-OA knee pathology and to optimize combination therapy protocols.
Read more about Hyaluronic Acid Injection for Knee here.
References
- Platelet-Rich Plasma Versus Hyaluronic Acid for Knee Osteoarthritis: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Belk JW, Kraeutler MJ, Houck DA, et al. The American Journal of Sports Medicine. 2021;49(1):249-260. doi:10.1177/0363546520909397.
- Patients With Knee Osteoarthritis Who Receive Platelet-Rich Plasma or Bone Marrow Aspirate Concentrate Injections Have Better Outcomes Than Patients Who Receive Hyaluronic Acid: Systematic Review and Meta-Analysis. Belk JW, Lim JJ, Keeter C, et al. Arthroscopy : The Journal of Arthroscopic & Related Surgery : Official Publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 2023;39(7):1714-1734. doi:10.1016/j.arthro.2023.03.001.
- Platelet-Rich Plasma Is More Effective Than Hyaluronic Acid Injections for Osteoarthritis of the Knee: A Meta-Analysis Based on Randomized, Double-Blinded, Controlled Clinical Trials. Li YF, Xing HH, Wei CK, et al. Arthroscopy : The Journal of Arthroscopic & Related Surgery : Official Publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 2025;:S0749-8063(25)00484-0. doi:10.1016/j.arthro.2025.06.033.
- Comparison of Hyaluronic Acid and Platelet-Rich Plasma in Knee Osteoarthritis: A Systematic Review. Xu H, Shi W, Liu H, et al. BMC Musculoskeletal Disorders. 2025;26(1):236. doi:10.1186/s12891-025-08474-6.
- Platelet-Rich Plasma Versus Hyaluronic Acid in the Treatment of Knee Osteoarthritis: A Meta-Analysis of 26 Randomized Controlled Trials. Tan J, Chen H, Zhao L, Huang W. Arthroscopy : The Journal of Arthroscopic & Related Surgery : Official Publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 2021;37(1):309-325. doi:10.1016/j.arthro.2020.07.011.
- Management of Osteoarthritis of the Knee (Non-Arthroplasty): Evidence-Based Clinical Practice Guideline. American Academy of Orthopaedic Surgeons (2021).
- The Efficacy and Safety of Intra-Articular Platelet-Rich Plasma Versus Sodium Hyaluronate for the Treatment of Osteoarthritis: Meta-Analysis. Liu Q, Ye H, Yang Y, Chen H. PloS One. 2025;20(3):e0314878. doi:10.1371/journal.pone.0314878.
- Platelet-Rich Plasma Combined With Hyaluronic Acid Improves Pain and Function Compared With Hyaluronic Acid Alone in Knee Osteoarthritis: A Systematic Review and Meta-Analysis. Karasavvidis T, Totlis T, Gilat R, Cole BJ. Arthroscopy : The Journal of Arthroscopic & Related Surgery : Official Publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 2021;37(4):1277-1287.e1. doi:10.1016/j.arthro.2020.11.052.
- Treating Knee Osteoarthritis With Platelet-Rich Plasma and Hyaluronic Acid Combination Therapy: A Systematic Review. Baria MR, Vasileff WK, Borchers J, et al. The American Journal of Sports Medicine. 2022;50(1):273-281. doi:10.1177/0363546521998010.
- Efficacy of Intra-Articular Injection of Combined Platelet-Rich-Plasma (PRP) and Hyaluronic Acid (HA) in Knee Degenerative Joint Disease: A Prospective, Randomized, Double-Blind Clinical Trial. Fossati C, Randelli FMN, Sciancalepore F, et al. Archives of Orthopaedic and Trauma Surgery. 2024;144(11):5039-5051. doi:10.1007/s00402-024-05603-z.
- Consensus Guidelines on Interventional Therapies for Knee Pain (STEP Guidelines) From the American Society of Pain and Neuroscience. Hunter CW, Deer TR, Jones MR, et al. Journal of Pain Research. 2022;15:2683-2745. doi:10.2147/JPR.S370469.
- Platelet-Rich Plasma, Bone Marrow Aspirate Concentrate, and Hyaluronic Acid Injections Outperform Corticosteroids in Pain and Function Scores at a Minimum of 6 Months as Intra-Articular Injections for Knee Osteoarthritis: A Systematic Review and Network Meta-Analysis. Jawanda H, Khan ZA, Warrier AA, et al. Arthroscopy : The Journal of Arthroscopic & Related Surgery : Official Publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 2024;40(5):1623-1636.e1. doi:10.1016/j.arthro.2024.01.037.
- Relative Efficacy of Intra-Articular Injections in the Treatment of Knee Osteoarthritis: A Systematic Review and Network Meta-Analysis. Singh H, Knapik DM, Polce EM, et al. The American Journal of Sports Medicine. 2022;50(11):3140-3148. doi:10.1177/03635465211029659.



